We all know that the drainage from HS can certainly be difficult to manage. The leaking and the weeping is unpredictable and often has different consistency, colour and odour. Typical HS lesions drain a lot, and usually this can be contained by an absorbent dressing like gauze, or absorbent pads like the HidraWear dressings. However, today we are going to talk about the more challenging aspects of hidradenitis suppurativa wound care.
Hidradenitis Suppurativa Wound Care
Sometimes HS lesions can develop into large open wounds that need more attention than usual. Or sometimes the skin that is trying to heal can go into overdrive. This can cause jelly like fleshy lumps to come out from the skin. This is called granulation tissue. In healthy wounds, it is flat and fills in the wound bed during the healing process. In some HS lesions, the body makes too much granulation tissue. This causes the tissue to grow above the wound bed and beyond the surface of the skin. This is called hypergranulation or over granulation. It can be caused by excess moisture, persistent inflammation, prolonged irritation or friction, or possible infection – all of which we sometimes see in HS wounds.
Hypergranulation in HS Wound Care
Hypergranulation can slow down wound healing, so it is important that if you notice pink or red fleshy tissue growing out from your skin to speak to your doctor or wound care nurse for advice, as these types of wounds cannot be managed by an absorbent dressing alone.
All granulation tissue is made by your body trying to heal. And sometimes HS lesions require more than an absorbent pad. Granulation tissue whether it is in a wound bed, or rising above the wound surface, should not be disturbed. Friction and inflammation can further slow down the healing process, so it is important to use a suitable primary dressing, and cover with a secondary dressing.
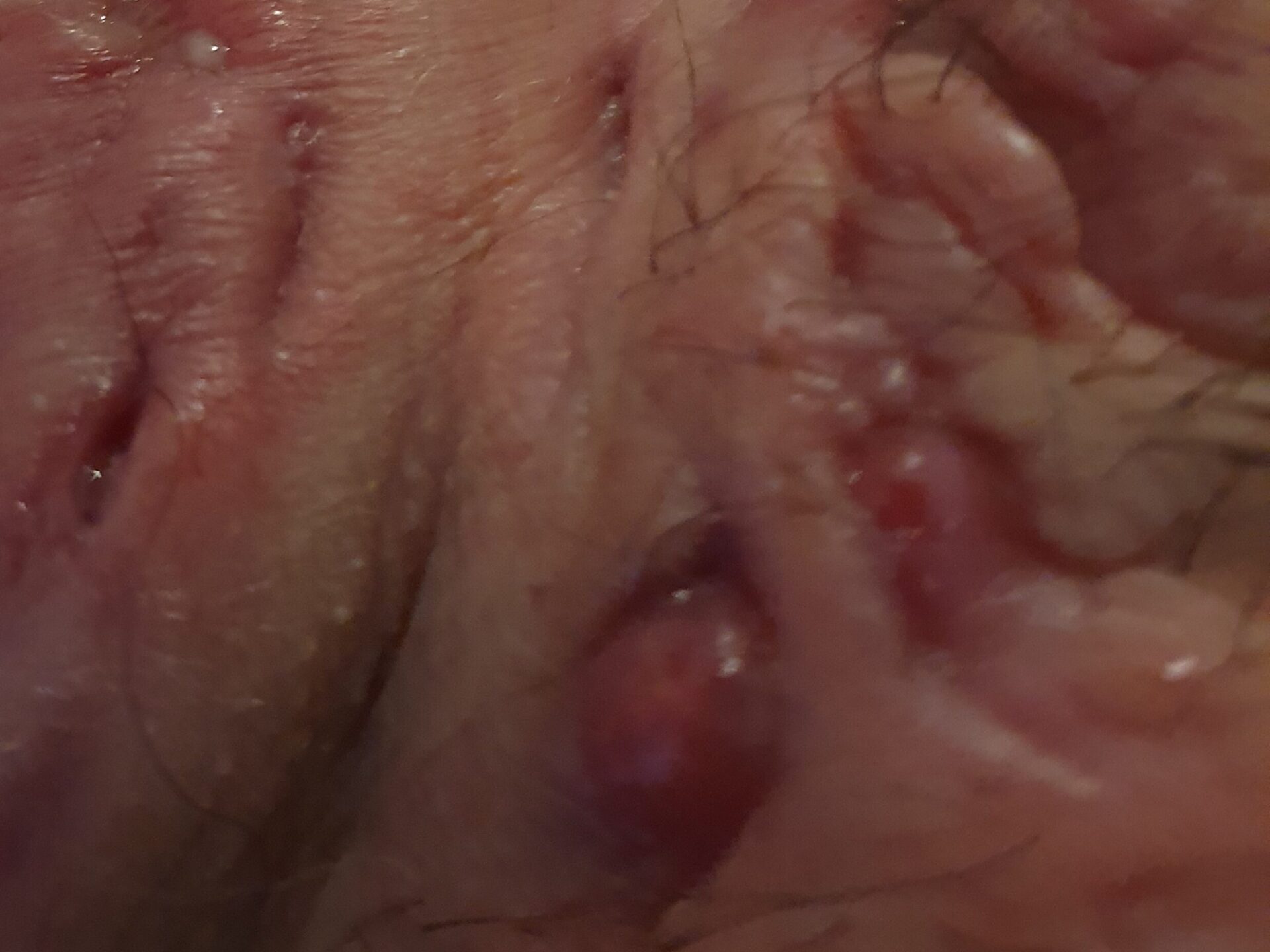
Hypergranulation – pink fleshy tissue can be seen rising above the surface of the skin.
An open wound requires a primary dressing
A primary dressing is a dressing that is placed directly on top of or into a wound.
A secondary dressing is a larger dressing placed over the primary to absorb any exudate, and to keep the primary in place.
Here is a helpful video demonstrating a dressing change
For HS wounds that are open or hyper granulating, very thin, soft flexible dressings are recommended as a primary dressing, that will not stick to the wounds. A secondary dressing could be the HidraWear dressing, or other dressings, like a mepore dressing, or a menolin dressing with adhesive tape, or other over the counter absorbent dressings.
Primary Dressings for Hidradenitis Suppurativa Wound Care
For a large open wound that is leaking/draining , you can try Aquacel dressings. They are very soft and turn to gel when drainage from the wound comes into contact with it, so there is no sticking or pain on removal.
Another option for an open wound, or hypergranulation tissue is a Mepital or adaptic touch dressing, which is a soft silicone layer that sits on the wound, protecting the new tissue, but allowing the drainage to flow through and into the secondary dressing. These primary dressings can be left in place for up to seven days, but you can change the secondary dressings as required. Always seek advice or refer to the manufacturers instructions on how to use these dressings.
The dressings above can be expensive to buy, so please speak to your doctor or wound care nurse to see if these are available to you on prescription or through health services. Your pharmacy may have to order these in for you.
Pharmacy Options for hidradenitis suppurativa wound care
If the dressings above are not an option for you, don’t worry. There are more primary dressings that are suitable and are available from most pharmacies.
Jelonet dressings are made of a very thin layer of gauze that has been coated with paraffin to prevent it sticking to the wound. These can be used on most HS lesions, but if you have a vey deep wound, these should not be used on them – please speak to your doctor and ask to be referred to a wound specialist.
Another primary dressing available from your pharmacy is an inadine dressing. It is a woven dressing, coated with a special ointment that contains iodine. Because this dressing has antimicrobial properties, long term use is not recommended, and it is recommended to use these types of dressings for 7-14 days, changing them as required. Please refer to the instructions on the packet.
Barrier Creams
If you cannot access any of these dressings, you can apply a barrier cream to the surrounding skin of the wound to prevent sticking. A barrier cream like cavillon, LBF or Relife can be applied in a vey thin layer. Please speak to your doctor or wound care provider about a suitable barrier cream for you. And make sure you read the information regarding application as they need time to dry before covering.
If you cannot access a barrier cream, you can use a very small amount of Vaseline, or sudocrem. Both of these are available in supermarkets.
Please remember, only a very small amount should be used. Too much barrier cream can clog pores and disturb the healing process. There should only be a very light sheen on your skin after applying.
Hygiene
The most important thing to remember when tending to your wounds is hygiene. Firstly, make sure you wash your hands, or use sterile gloves if you have them. Also ensure any equipment like scissors or mirrors are clean before you start your wound care.
So if in doubt, please speak to your doctor. You don’t have to go this alone. If you have an open wound that you are finding difficult to manage, take action. Ask to be referred to a wound expert to assist you with your wound management.
This article was medically reviewed by Kerry and Karen, advanced wound care practitioners and wound care educators.
If you found this article helpful, you can register for our newsletter to receive articles and blogs.